Tension Pneumothorax
 - One way valve leak. Air is pushed into the pleural space with no means of escape, so collapses the affected lung.
- One way valve leak. Air is pushed into the pleural space with no means of escape, so collapses the affected lung.- The mediastinum is displaced to the opposite side.
- Most common cause is mechanical ventilation.
- Signs include chest pain, air hunger, respiratory distress, tachycardia, hypotension, tracheal deviation AWAY from the side of injury, unilateral absence of breath sounds, elevated hemithorax, neck vein distension, cyanosis.
Classic signs of
tension pneumothorax
tension pneumothorax
| Trachea | ||
| Expansion | ||
| Percussion Note | ||
| Breath sounds | ||
| Neck veins |
Thoracocentesis
5cm needle will reach the pleural space >50% of the time
8 cm needle will reach the pleural space >90% of the time.
Procedure - ATLS Way
- Assess chest and respiratory status
- Administer oxygen and ventilate as necessary
- Identify 2nd intercostal space, midclavicular line
- Surgically prepare the chest. Local anaesthesia if time permits.
- Place patient upright if c-spine injury has been excluded.
- Insert a catheter into the skin, and direct the needle over the rib into the intercostal space.
- Puncture the parietal pleura.
- Remove the needle. Replace the leur lock. Dress.
- Prepare for chest tube insertion
Complications: Local haematoma, pneumothorax,lung laceration, failure
- Placing the needle medially increases the risk of damage to the internal mammary vessels and mediastinum. Lots of experienced ED physicians demonstrated their placement was far too medial.
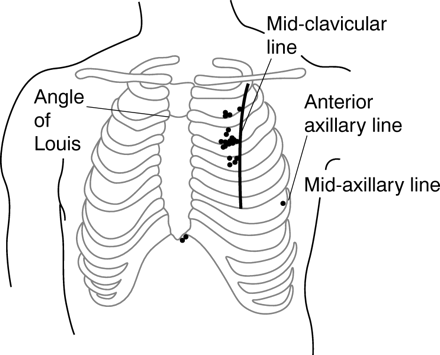 |
| Emerg Med J 2005;22:788–789 |
Discussion Points
- Cannula - lots of discussion about the length of the cannula. In the UK the cannulas we use seem to be quite short compared to other options. Normal IV cannulae do not reach in up to 65% of cases.
- Some places suggest adding a syringe of saline to the cannula so you can see the bubbles as you go. The cannula can also get easily blocked or kinked.
- CXR first? - recently been called into question. Difficult to know if needle has reached pleura, so a CXR can be helpful. If there is no haemodynamic compromise, wait for a chest x-ray. If there is compromise, do not delay.
Leigh-Smith and Harris recommend urgent CXR first in awake patients, except when:
SpO2< 92% on oxygen
Systolic BP< 90 mmHg
Respiratory rate <10
Decreased level of consciousness on oxygen
Cardiac arrest
- Misdiagnosis?
If you think a patient has a pneumothorax, you decompress the chest, and don't hear hiss and the patient doesn't improve, and the CXR shows no pneumothorax - do you still need a chest drain? There's no evidence either way - follow local guidelines.
- Tension gastrothorax has similar symptoms. It is caused by a diaphragmatic tear.
References
http://lifeinthefastlane.com/ccc/emergency-thoracocentesis/
http://emj.bmj.com/content/22/11/788.full
http://emj.bmj.com/content/19/2/176.full
http://journal.publications.chestnet.org/article.aspx?articleid=1060258
http://www.trauma.org/archive/thoracic/CHESTtension.html
http://intensivecarenetwork.com/download/emergency-thoracocentesis-doc/
http://emcrit.org/podcasts/needle-finger-thoracostomy/
http://bestbets.org/bets/bet.php?id=783
http://emergencymedicineireland.com/2012/11/stop-putting-iv-cannulae-in-the-2nd-ics-for-tension-ptx/
Emerg Med J 2005;22:788–789


No comments:
Post a Comment